By law, hospitals must notify patients that they may incur substantial out-of-pocket costs if they remain in the hospital for more than 24 hours without formal admission.
But in the bustle and confusion, hospital status isn’t always clear enough to help you make informed decisions.
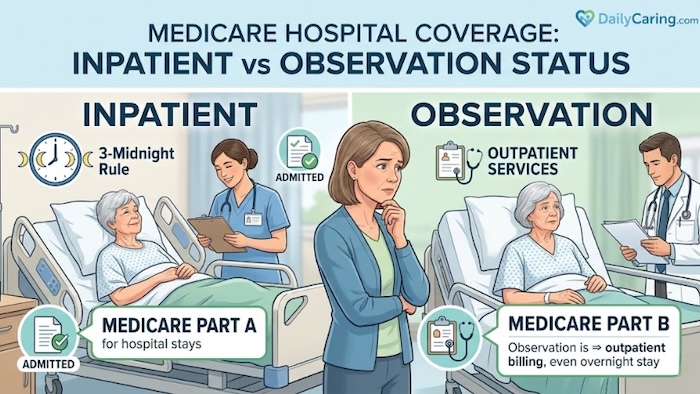
We explain the difference between Medicare inpatient vs. observation status, how Medicare coverage for hospital stays works, how hospital status affects coverage for nursing home stays, and what seniors should expect to pay under each status.
Medicare Inpatient vs Observation Status at the Hospital
A hospital classifies a patient’s status as either inpatient or observation.
Having an inpatient status means that the person has been admitted to the hospital under a doctor’s orders.
Being in observation status means the person is staying in the hospital as an outpatient. They haven’t been admitted.
Please don’t assume that you know your older adult’s status based on what procedures are being done or how long they’ve been in the hospital.
And remember, staying overnight or for many days doesn’t mean that someone has been admitted.
Medicare Coverage is Based on Hospital Status
Hospital status determines the Medicare coverage for hospital stays and post-hospital care.
There are separate coverage rules for inpatient and outpatient hospital stays. Typically, out-of-pocket costs are significantly higher for outpatient stays.
The difference between an inpatient and outpatient stay could mean thousands of dollars out of your older adult’s pocket.
The timing of admission is also essential, as Medicare covers only the inpatient portion of a hospital stay.
Any time spent in the hospital or emergency room before admission is considered outpatient time.
That time is covered under outpatient coverage rules and doesn’t count toward the 3-day minimum for covered skilled nursing care.
It’s also important to know that the discharge day doesn’t count as an inpatient day.
VIDEO: What You Need to Know About Medicare Hospital Billing
How Hospital Status Affects Coverage for Short-Term Nursing Home Stays
When an older adult is hospitalized, a common next step is for them to be discharged to a nursing home (skilled nursing facility) for rehab and further recovery.
However, Medicare coverage for these short-term nursing home stays depends on the hospital's status.
To be eligible for coverage, a person must have 3 hospital inpatient days. Otherwise, they’ll be responsible for the cost of the skilled nursing facility stay.
For a real-life example, imagine that your mom got very ill and has been in the hospital for 5 days.
When the hospital is ready to discharge your mom to a skilled nursing facility, you suddenly find out that Medicare won’t cover any of the cost.
Typically, Medicare covers short-term nursing home stays after a hospitalization. So why wouldn’t Medicare cover the nursing home in this case?
It turns out that your mom was never admitted to the hospital by the doctor, so she didn’t have inpatient status and had zero inpatient hospital days.
She didn’t have a “qualifying hospital stay” because she was an outpatient under observation status.
Because of this status, your mom’s hospital costs will now be determined under the rules for outpatient coverage, and she’ll also be responsible for the price of the nursing home stay.
Inpatient vs Observation Status: What Seniors Should Expect to Pay
What seniors pay as inpatients:
- For the first 60 days of hospital services, pay the Part A deductible.
- For a doctor’s services (typically), pay the Part B deductible + 20% of the Medicare-approved amount.
- For nursing home/rehab care, if the inpatient hospital stay was at least 3 days, only pay after the first 20 days (fully covered) in an approved skilled nursing facility.
- Get more details about inpatient hospital stay coverage at Medicare.gov
What seniors pay as outpatients (observation status):
- For hospital services, pay a copayment for each outpatient hospital service. This amount may vary by service.
- For doctors’ services, pay the Part B deductible + 20% of the Medicare-approved amount.
- For prescription and over-the-counter medications in the hospital or emergency room, pay out-of-pocket (and try to submit a claim to the drug plan later) or try to use Part D prescription drug coverage.
- For nursing home / skilled nursing rehabilitation care, pay out of pocket.
- Get more details about outpatient coverage at Medicare.gov
Comparison Table: Medicare Inpatient vs. Observation Costs
Because the financial impact of your hospital status can be significant, it helps to see the costs side-by-side. Use this quick-reference chart to compare how Medicare Part A and Part B handle hospital services, medications, and skilled nursing care.”
| Feature | Inpatient Status | Observation Status |
|---|---|---|
| Medicare Coverage | Part A (Hospital Insurance) | Part B (Medical Insurance) |
| Hospital Deductible | One-time Part A Deductible | Part B Deductible + 20% Copays |
| Medications | Covered by Part A | Often Out-of-Pocket / Part D |
| Rehab/Nursing Home | Covered (after 3 midnights) | NOT Covered |
| More Info | View Part A Details | View Part B Details |
Final Thoughts About Medicare Hospital Billing
Understanding the distinction between inpatient and observation status is one of the most critical steps in managing Medicare costs.
While a hospital stay may look the same from a patient’s bedside, the administrative classification dictates whether thousands of dollars in nursing home rehabilitation or hospital co-pays will be covered.
By staying proactive, asking the medical team for a formal status update daily, and understanding the “3-midnight rule,” you can better advocate for your loved one’s health and financial well-being.
Disclaimer
This article is for informational purposes only and does not constitute medical, legal, or financial advice. Medicare policies and hospital regulations are complex and subject to change. Always consult with a qualified professional, such as a Medicare specialist or healthcare provider, regarding your specific situation before making healthcare or financial decisions.
Recommended for you:
- What Does Medicare Cover? Find Out Before the Bills Arrive
- Medicare vs. Medicaid: What You Need to Know
- Get Help with Medicare Questions from State Programs
About the Author

Connie is the founder of DailyCaring.com and was a hands-on caregiver for her grandmother for 20 years. (Grandma made it to 101 years old!) She knows how challenging, overwhelming, and all-consuming caring for an older adult can be. She also understands the importance of support, especially in the form of practical solutions, valuable resources, and self-care tips.















From a selfish perspective I am especially interested in the charges I will have to pay after my Medicare Supplement makes their payment. I have Supplement F. Is their a table that breaks down my anticipated charges according to the supplement and the inpatient/outpatient circumstance (as your excellent article did pre-insurance)?
It would be best to contact your insurance company to find out what the out-of-pocket costs will be for your specific situation.
Having just enountered this situation in the Main Line Health system in suburban Philadelphia that’s evolved into a quality control review case, I will say that hospitals can play fast and loose with the definition of “observation.” It is not observation if a patient is brought into the ER, kept for up to a week, has repeated episodes of a medical problem during that period and the hospital is unable to treat or manage it. The three-day rule is plain: If a hospital is incapable of keeping the patient’s problem under control for three days, then the patient needs to be admitted. Whether that inability is due to doctor’s skill set, the severity of the patient’s problem or whatever, admission is required.
But let’s be blunt. A hospital will bring in much more revenue from billing on outpatient charges than inpatient. Also, if a patient is readmitted with the same problem within a defined period of time – meaning the hospital didn’t effectively treat the problem – Medicare does not pay for the second round of treatment. But if the patient’s first go-round was on observation status, that doesn’t count as admission so hospitals don’t risk Medicare non-payment.
A law alerting patients is great. But if hospitals don’t honor their end of the bargain, it means nothing.
I’m so sorry you have to go through all this 🙁 Hospitals do have a lot of things they can do to charge patients more. That’s why it’s so important for seniors to have a strong health advocate to make sure they’re getting fair treatment and accurate bills.