Managing mealtime for a loved one with swallowing difficulties can feel like a high-stakes balancing act. When a simple sip of water or a bite of dinner poses a risk of choking or infection, the joy of eating can quickly turn into a source of anxiety for both the senior and the caregiver.

This guide walks you through the essentials of dysphagia management, providing the tools you need to restore safety, nutrition, and dignity at every meal.
Understanding Dysphagia: More Than Just “Trouble Swallowing”

Dysphagia isn't just a minor inconvenience; it's a serious medical condition in which the muscles and nerves involved in swallowing don't function properly.
For many aging adults, this results from the natural weakening of muscles, but it is often linked to underlying conditions like Parkinson’s disease, Alzheimer’s, or the aftermath of a stroke.
Understanding the “why” behind the difficulty is the first step in creating a safe environment.
The Hidden Danger of Dysphagia: Silent Aspiration

The most significant risk associated with dysphagia is aspiration (when food or liquid enters the airway and lungs instead of the stomach). Most concerning is silent aspiration, in which a senior may inhale food without any obvious signs, such as coughing or choking.
Over time, this can lead to aspiration pneumonia, a leading cause of hospitalization for seniors with swallowing disorders.
Getting a Professional Diagnosis for Dysphasia
If you notice signs such as frequent throat clearing, a “wet” voice after eating, or unexplained weight loss, it’s time for a professional assessment.
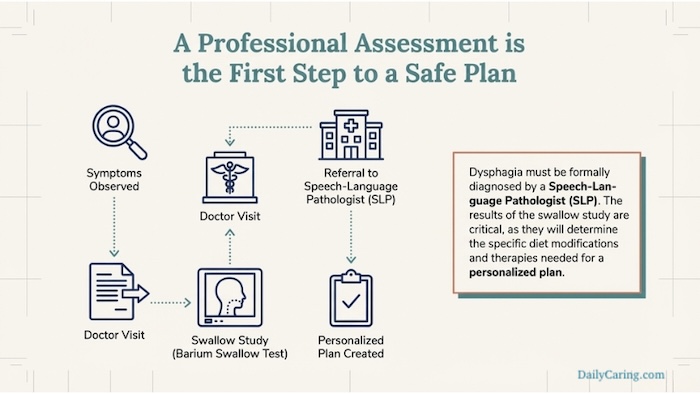
A Speech-Language Pathologist (SLP) is the primary expert in this field. They will often perform a Video Fluoroscopic Swallow Study (VFSS) or a Fiberoptic Endoscopic Evaluation of Swallowing (FEES) to see exactly what is happening during the swallow and recommend a specific personalized care plan.
VIDEO: Managing Dysphagia in Aging Adults
Managing Dysphagia: The 3 Pillars of Care
Once you have a professional diagnosis and a personalized care plan from an SLP, the path forward is organized into three primary areas of focus. Think of these as the “Three Pillars” of dysphagia management. Together, they form a comprehensive safety net:

- Dietary Modification (adapting what is eaten)
- Safe Swallowing Techniques (adapting how one eats)
- Strength and Coordination Exercises (rehabilitating the swallow itself)
By balancing these three pillars, you can significantly reduce the risk of aspiration while ensuring your loved one receives the hydration and nutrition they need to stay strong.
Pillar 1: Mastering Diet and Texture Modification in Dysphagia
The cornerstone of dysphagia safety is modifying what your loved one eats and drinks. We use the IDDSI Framework (International Dysphagia Diet Standardization Initiative) to ensure consistency.
Managing Liquids When It Comes to Dysphagia

These are categorized from Level 0 (Thin) to Level 4 (Extremely Thick). Thickening agents help slow down the flow of liquid, giving the throat muscles more time to react.
Managing Foods When It Comes to Dysphagia

Textures range from Pureed to Soft & Bite-Sized. It is critical to avoid “transitional” foods like ice cream or gelatin, which can melt in the mouth and become a dangerously thin liquid before they are swallowed.
Boosting Nutrition and Hydration is Important When Dealing with Dysphagia

Seniors with dysphagia are at high risk for malnutrition and dehydration because eating becomes a chore. To combat this:
- Focus on nutrient-dense purees (like squash, avocado, or Greek yogurt).
- Use flavor enhancers (stronger spices or herbs) to stimulate appetite.
- Offer smaller, more frequent meals throughout the day to prevent mealtime fatigue.
Pillar 2: Safe Swallowing Techniques

How a person eats is just as important as what they eat. Implement these “safe-swallow” habits:
- Upright Posture: Ensure they are sitting at a 90-degree angle during and for 30 minutes after meals.
- Slow Pace: Use a small spoon to control bite sizes and ensure the mouth is clear before the next bite.
- No Straws: Straws often deliver liquid too quickly to the back of the throat; sipping from a cup is usually safer unless an SLP advises otherwise.
Managing Medications in Dysphagia

Pills are often the most difficult things to swallow. Discuss with your pharmacist whether medications can be:
- Crushed and mixed with a spoonful of applesauce or pudding.
- Converted to an oral suspension (liquid form) that can then be thickened to the appropriate IDDSI level.
Note: Never crush “extended-release” or “enteric-coated” tablets, as this can be dangerous.
Pillar 3: Strength and Coordination Exercises
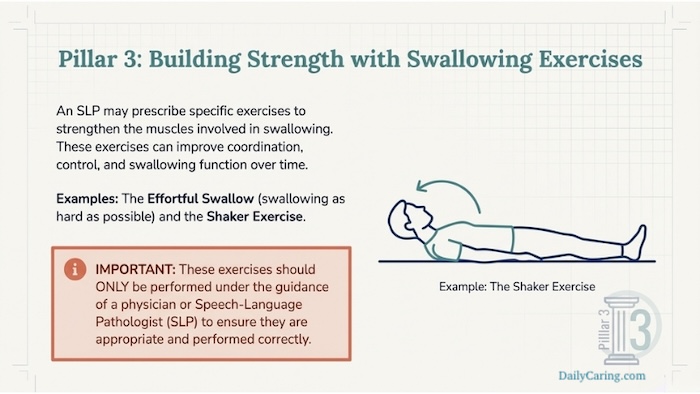
While you should never attempt these without guidance, an SLP may prescribe specific exercises to strengthen the swallowing mechanism. Techniques like the Effortful Swallow or the Shaker Exercise are designed to improve muscle coordination.
Think of these as “physical therapy” for the throat, helping to rebuild the ability to protect the airway.
The Caregiver's Role in Dysphagia: Advocate, Coach, and Observer

As a caregiver, you are the front line of defense. You are the observer who notices a change in swallow patterns, the coach who encourages safe techniques, and the advocate who ensures every member of the healthcare team (from the doctor to the home health aid) is following the established safety plan.
Your vigilance preserves not just their health, but their quality of life.
Dysphagia Red Flags: When to Seek Out Help
Red Flags: When to Seek Immediate Help
If you notice any of the following symptoms, contact a healthcare provider or a Speech-Language Pathologist immediately.
- ▲ Unexplained weight loss
- ▲ Recurrent chest infections or pneumonia
- ▲ Persistent coughing, choking, or gagging during or after meals
- ▲ A wet or “gurgly” sounding voice after swallowing
- ▲ Pain during swallowing
Dysphagia Resources and Support
You Are Not Alone: Resources & Support
Managing dysphagia is demanding. It’s vital to protect your own well-being and connect with others for support and information.
Final Thoughts on Dysphagia: Restoring the Joy of the Meal
Managing dysphagia is a journey that requires patience, vigilance, and a dedicated heart. While the clinical aspects (like IDDSI levels and swallow studies) can feel clinical and overwhelming, the ultimate goal remains deeply personal: ensuring your loved one can eat safely while maintaining their dignity and quality of life.
By leaning on the “Three Pillars” and staying alert for red flags, you aren't just managing a medical condition; you are protecting the simple, essential joy of a shared meal.
Remember, you don't have to navigate this alone; reach out to professionals and community resources to help you and your loved one thrive.
About the Author

Chris is a seasoned healthcare executive and entrepreneur from the Pacific Northwest. He strongly advocates for older adults and the caregivers who serve them. Chris has personal experience caring for his father, who had dementia. Chris is a technology enthusiast and an avid outdoorsman; if he's not in his office, he can usually be found on a golf course or fly-fishing out west somewhere.














